Bird flu has been back in the news with several scare headlines lately. Among the most prominent last week were the announcement of the first ever human case in Australia, and a human case in the United States. The stock tickers for numerous vaccine makers popped — some of which actually make flu vaccines.
No, you should not be worried about either of those cases. We’ll get to that later.
However, if just those headlines are causing knee jerk moves of millions of dollars again, it’s probably time for a quick review of bird flu—with my own opinions, as usual.
You will see bird flu called a few different things, besides “bird flu.” You may see “avian influenza virus” (AIV) or “highly pathogenic avian influenza virus” (HPAIV) when they want to really get some emotion out of you. They all refer to the same thing, which is a family of influenza A viruses that are really good at causing high mortality flus in birds.
The family of bird influenza viruses in recent news (typically the H5N1) has been around for 40-50 years at this point. Bird flus overall have been around for much longer. This is not a new thing, by any stretch of the imagination. During that period, there have been numerous small outbreaks and clusters where H5N1 or H7Nx etc. virus has managed to infect humans, and they have caught the bird flu. We’ll get into the epidemiology of that shortly. Human-to-human transmission has been very rare, if happening at all, and typically no more than a case or two when it has happened in that span.
As we mentioned late in the coronavirus updates, a particular strain of bird flu was making news because it was crossing over to more and more mammalian species. The H5N1 version of bird flu has been mostly responsible for this. The species leap is what has infectious disease experts a little more nervous, and “POSSIBLE DOOMPLAGUE! WILL YOUR FRIENDS AND FAMILY DIE HORRIBLY NEXT?!?!?!” always drives clicks on otherwise slow news days.
“So,” I hear you ask, Appropriately Headline Cautious After COVID Hypothetical Reader, “how much of a risk is this H5N1 thing anyways?”
That’s what we’ll get into!
But first, we need to start with the very basics of influenza A, and how flu does what it do.
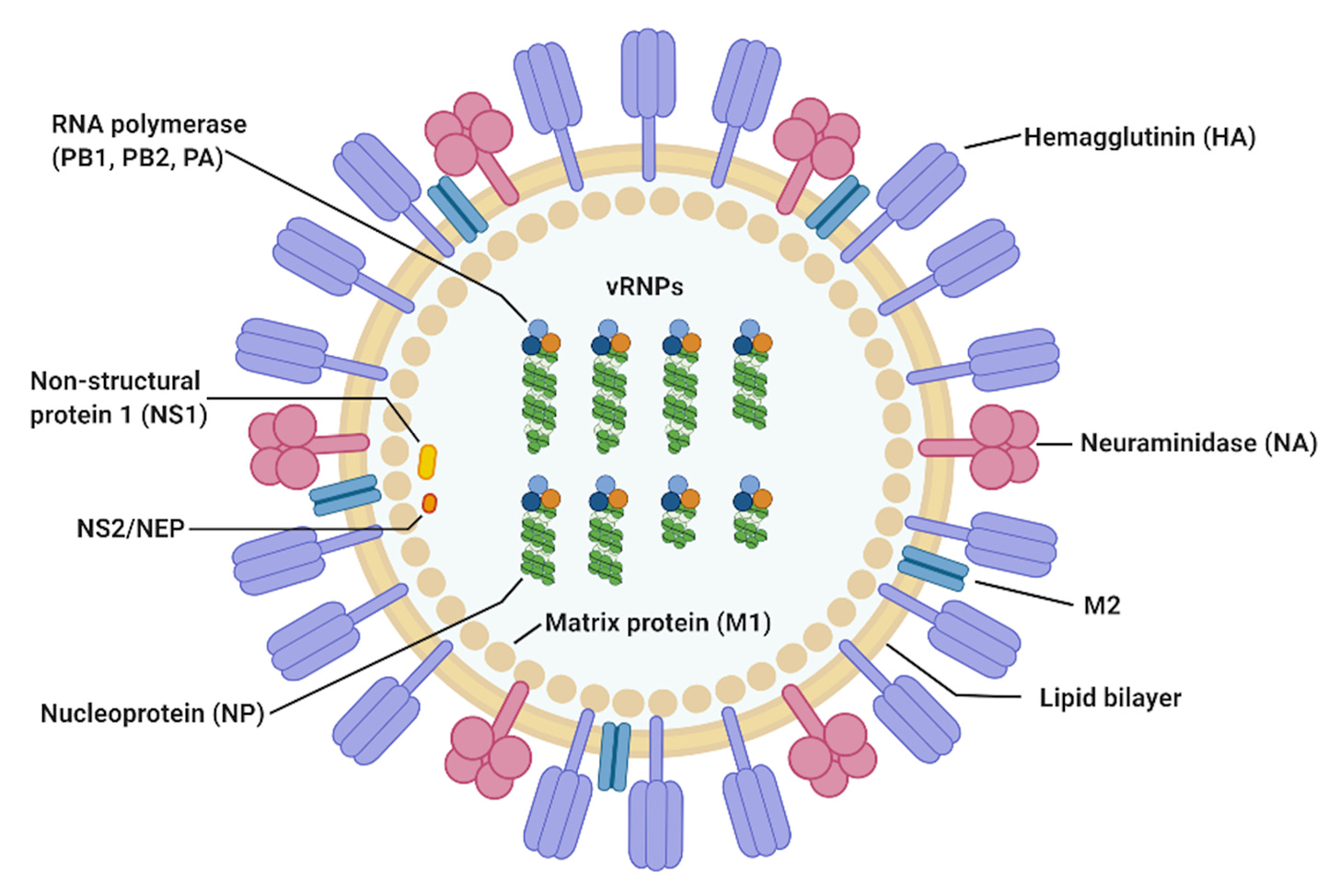
This is a diagram of influenza A available via Creative Commons so I can be really lazy and just use it here:
By Hi Eun Jung and Heung Kyu Lee - https://www.mdpi.com/1999-4915/12/5/504/htm, CC BY 4.0, https://commons.wikimedia.org/w/index.php?curid=92944856
The yellow circles are the virus capsid, or the outer protein shell of the virus. You will notice it has a lot of blue and red “clubs” sticking out of it — these are important flu proteins. The blue clubs are called hemaggluttinin and the red are neuraminidase. We will call these “H” and “N” respectively, and yes, Astute Hypothetical Reader, those are the same H and N that give a particular flu strain its “HxNy” designation — like the H5N1 avian flu.
All “H5N1” says is that this particular flu strain uses an H protein in the “5” family of H proteins, and a N protein in the “1” family of N proteins.
H is used by the influenza virus to bind to receptors on the cells they will infect. For flu, these receptors are actually modified sugars that coat your cells. That’s not as important as knowing the “H” is what flu uses to break into your cells — particularly your respiratory cells. But H can also grab onto modified sugars on your red blood cells too, which is how it gets its long “hemeaggluttinin” name, which is science for “causes red blood cells to stick to each other” because if the virus uses H to grab more than one red blood cell at a time, it will cause them to stick to the virus and thus each other with the virus as a bridge between them.
So let’s talk about a day in the “life” of a flu virus. The virus floats through the air in a droplet, doing nothing. Lucky for the virus, the droplet is inhaled by some critter. The droplet is drawn deep into the critter’s lungs until it lands on the respiratory cells there. As the droplet bursts on impact, our virus particle is released.
The H on flu’s surface grabs the respiratory cells of the critter’s lungs by those modified sugars, and holds on tight.
And now flu goes full-on terrorist…-Jedi- terrorist…
Like Old Ben Kenobi distracting you from what are clearly the droids you are looking for, the virus convinces the respiratory cell that it’s not really a virus. Probably something tasty for the cell, conveniently stuck to the respiratory cell’s surface.
Yes, the respiratory cells buy this, because they are weak-minded fools when it comes to Jedi mind tricks. Or maybe they just like snacks a little too much. Either way, they pull the virus into the cell, the exact thing the virus wants, and we critters do not.
Influenza A in hacker voice: “We’re in…”
(original creation via DALL-E3 model on NightCafe)
Now inside the cell, it’s hijackin’ time for the virus. An intricate dance of viral proteins starts to cut the virus out of the transport bubble the cell used to bring it in. This eventually leads to the virus’ genome being released into the cell, where the genome is taken straight to the nucleus.
Inside the nucleus, the viral genome “borrows” the replication machinery for your RNA and DNA to make as many copies of itself as it possibly can. So in the nucleus, many more copies of the viral genome are made. Meanwhile, flu virus mRNA starts to hijack your ribosomes, causing them to make all the proteins for the outer shell of the virus. So new H and N proteins, all the structural proteins and a few non-structural proteins the virus carries.
The non-structural proteins of flu A, including bird flu, are used to block your immune system as much as possible. Simplified a bunch, bird flu non-structural proteins appear to have two key functions — blowing up the antigen-presenting cells and making cytotoxic T-cells less effective. Think of the antigen-presenting cells as an alarm system — they let B-cells and T-cells in your immune system know something is breaking in AND show pieces of it so B-cells can make antibodies and T-cells can hunt down virus-infected cells. The cytotoxic T-cells are the varsity-level “Among Us” players. Their job is to hunt down “imposter” cells infected with viruses and vote them off the space ship to eliminate them — just like in the game your kids play with their friends.
So TL;DR, the non-structural proteins of bird flu turn off key immune system alarms and make your T-cells -worse- “Among Us” players, so the virus, the “imposters” can “win” more often.
Meanwhile, the new viral genomes are going to be loaded into the new viral protein shells being made inside the infected cell. Once the new virus particle is complete, it heads back to the surface in a transport bubble. Now it’s the N protein’s time to shine, as the “N” part of the virus is used to cut the virus free of the surface of the cell once transport bubble gets there. So many virus particles can be released at once that they literally destroy the host cell.
The flu doesn’t care. It’s here for a good time, not a long time.
The new flu virus particles now go on and try to infect another cell, and start the whole process over and over again. Some of them will find nearby cells in the critter’s lungs. Others will be exhaled as droplets, in coughs and sneezes, to try to infect entirely new hosts.
Remember, a perfectly evolved virus wants to get in, replicate as much as possible, and get back out again — without ever alerting your immune system that it was there.
And this is the best DALL-E3 did asking for “Ethan Hunt from Mission Impossible with an influenza A particle for his head.”
Viruses which we call “highly pathogenic” are really just bad viruses, where there is an evolutionary mismatch between us and them. Most of the symptoms you associate with the flu are actually your immune system responding to kill the virus. Flu tends to kill by massive viral replication with massive damage to the lungs called "diffuse alveolar damage" with “acute respiratory distress syndrome” as part of the viral pneumonia, and/or massive immune response causing “sepsis” and multi-organ failure from a combo of viral damage and off-target massive immune reaction.
Again, the best way to think of “sepsis” is the Ah-nold effect we discussed in COVID. If you need a reminder of this effect, you can find one here.
Viruses don't "want" to do this -- it's bad for the replication business. This is also why, in general, over a pandemic or epidemic, the virus will mutate to become more contagious but less severe. Over a pandemic, it becomes harder to find susceptible hosts and the virus has a better chance to do that by becoming “sneakier.” The only alternative is to become so contagious that the virus can rapidly find new hosts even as the old ones die — but this is ultimately self-defeating for the virus. Kill all possible hosts, and the virus will not replicate no mo' either. The only thing a virus ever wants to do is make more of itself. Even if not lethal, a virus that gets more severe, causing serious illness, tends to cause host organisms to “social distance” to avoid getting seriously sick — and as we saw during COVID, that absolutely slaughtered the flu, with some pretty mild seasons at the height of social distancing.
So that’s the short version of flu virology, and what it "wants" to do with this process.
However, we need to pause in our story of viral nefariousness, because the influenza A virus genome is worth taking a moment to discuss.
The way influenza A structures its genome (plus its often great contagiousness), and the consequences of that structure, is why this virus family is -THE- top viral pandemic threat.
Influenza viruses keep their genome in 8 separate little pieces. Yes, this is very similar to chromosomes, which are 46 separate pieces of DNA that make up your genome (23 from Mom and 23 from Dad, which is how “23andMe” got its name). In fact, keep that thought in mind that you half of your chromosomes from one parent and half from the other. Things don’t work quite the same for influenza A — but because the virus genome is in chromosome like pieces, you CAN get different entire “chromosomes” from different “parent” flu viruses if they are replicating in the same cell at the same time!
“Wait, does that ever happen? Can the same cell have multiple different flu viruses hijacking it at the same time?” I hear you ask, Hypothetical Reader.
Yes. At the height of flu seasons, and especially for those who work on farms with lots of birds and animals, it absolutely can happen. For example, a cow hanging out near the chicken coop on Old MacDonald’s farm may catch bird flu H5N1 and a more cow-specific flu virus (say, H3N2) at the same time. The bird flu may suck at replicating inside the cow cells (and often does—more on that in a minute), but it doesn’t need to be great at replicating for disaster to happen.
What disaster? Glad you asked!
In our hypothetical dual-infected cow cell, the bird flu H5N1 virus has just barely managed to make it inside and now sends 8 genome pieces to the nucleus. There it discovers a H3N2 cow flu virus is already merrily replicating away. As the cow flu virus is packing up new virus particles to leave, it’s not paying very close attention to which flu genome fragments it is loading up. So a new flu virus particle is loaded with 7 cow flu genome fragments and 1 bird flu fragment. Perhaps this changes the new virus to H5N2, as a Frankenflu is formed with the bird flu “H5” gene and everything else coming from the cow flu.
This is called “genetic shift” in flu viruses, and these Frankenflus can make huge leaps. Because now this H5N2 Frankenflu in the cow is exhaled near the chickens. The “H” part of it makes this bird flu really great at getting into chicken cells — after all, that H5 came from a bird flu. But all the rest of that flu grew up in cows. Remember how we said viruses that are not well adapted to their hosts can sometimes be really nasty viruses with unexpected toxicity and a massive immune response? Well, that’s what happens here, and the birds catch a really nasty flu from this naturally gene swapped Frankenflu. On top of that, it’s unlikely the chickens have seen the cow version of “N2” before, so part of their problem is their immune system has to start from square 1 making antibodies to that.
Flu is also an RNA virus, and those have a slightly higher mutation rate in their own right. This is usually more responsible for epidemics rather than pandemics, as these slight changes might let a flu get past a vaccine by looking just different enough. Or it can tweak the bird flu “H5” just enough that instead of being unable to bind human cells at all, it can start to. Then if it gets into a human cell, when a human flu is also there, and some Frankenflus get formed…
You get the picture.
So why are we suddenly all worried about bird flu? Well, it’s not sudden. Medical scientists have been worried about bird flus for awhile — and there is a huge amount of research on them already. Some of them are just really nasty to birds, with highly contagious and severe flus that can kill a lot of chickens and wild birds. To contain a nasty bird flu, chickens and turkeys at the same farm as an infected bird all must sometimes be euthanized to protect wild birds and birds at farms down the road.
In some outbreaks, this has resulted in millions of birds being put down or outright killed by flu.
But bird flus have shown an annoyingly high rate of leaping to other species as well. Birds also migrate enormous distances, helping spread these flus and provide themselves new chances to hop species. Over the past several years, they have been found in many other mammals, such as thousands of ferrets near the end of COVID, to a shockingly large number of cows here recently. The concern is that a bird flu hops a species and creates a Frankenflu that maintains the same nastiness it has for birds.
Hyping that concern is that over the past 40 years, a little under 900 people worldwide have been infected by bird flus that jumped over to humans and caused a flu. The case fatality rate for those 900 patients is reported to be up to 60%.
“SWEET BABY COVID, THAT’S WORSE THAN THE BLACK DEATH! THAT’S EBOLA MORTALITY WITH THE CONTAGIOUSNESS OF FLU! THE HEADLINES ARE RIGHT — WE ALL GONNA GET DOOM FLU!!!!!” I hear you all caps yell Hypothetical Worried Reader.
Yeah, we’re going to pump the brakes on that 60% CFR a lot. The true case fatality rate is, without question, MUCH lower. How much lower? No idea. But it’s a LOT lower than 60% — of that I am sure. Were I handicapping a possible bird flu pandemic, odds are still best that it would be a really bad flu season (so ~COVID equivalent) or less. Small chance (but not zero) it hits Spanish Flu levels, but that would pay out big in Vegas if it hits.
Why am I “back of the enveloping” those odds?
The reason true case fatality rate of these cross-over bird flus is way lower than 60% comes down to the testing used to confirm the flu infection.
Only symptomatic patients were tested. In some cases, only post-mortem testing, trying to figure out why this person got a terrible pneumonia and died.
Even in places that had an impressive, country-wide screening system in place, like a 2018 publication from Egypt, only patients with symptoms of flu were screened, and only at designated centers of excellence.
The odds are overwhelming that many people who work closely with birds are getting exposed to these bird flus. But we know from the 40 years worth of lab work on bird flus that their “H” protein (the one needed to get into a cell) looks for a particular bond in sugars that birds have in abundance — and human sugars don’t really use. We do know from lab studies that it can take as few as four genetic drift mutations (small ones, not swapping genome fragments) to get a bird flu H to start binding human respiratory cells in petri dishes. But we know from those same lab studies that when they get into human cells, they still don’t replicate very well.
Consistent with this, in 40 years and ~900 patients worth of bird flu, hardly any of those infected patients got their flu from another human. All had some form of contact with birds — the vast majority were involved in chickens and chicken processing.
That sounds more like really unlucky humans who caught a bird flu just strong enough to replicate in them, but not great at infecting other humans overall. So we might expect a lot of people exposed to bird flus, but never developing any symptoms whatsoever.
You can also see signs of this in the recent scare headlines. Remember just a few weeks ago when bird flu H5N1 was found in up to 20% of milk samples sent for pasteurization in the US?
Remember the curious incident of the cows in the night in those articles?
“What curious incident of the cows in the night? There was no massive amount of US cows with flu symptoms from the bird flu, let alone dying of flu, that we would expect from 20% of cows having H5N1 detectable in their milk. The cows did not moo in the night at all!” I hear you say, Hypothetical Elementary Dear Watson Reader.
Yes — that was the curious incident of those cows with the bird flu. No reports of cows with the flu alongside the detection of H5N1 in milk. No sudden explosion of flu in cattle workers. But at least 1 in 5 cows may have been carrying an H5N1 bird flu. Curious, no?
The best explanation is that H5N1 bird flu was just good enough at getting into cows to replicate a little but not really cause symptomatic flu in them. Many of the tests on the milk were done with PCR, which detects as little as a few copies of the virus in the milk. I am not aware of anyone reporting quantitative results of this milk screening, estimating how many copies per cow were there. Only qualitative. One can read headlines blaring that “20% of the milk has H5N1 bird flu in it!” and think that 1 in 5 gallons is just teeming with virus. Not necessarily true, and very likely not true! Extremely sensitive PCR may just be showing a lot of cows have been exposed to a H5N1 bird flu, which is probably replicating a little in them (given its prevalence) — but only a little, since we don’t have a massive symptomatic outbreak of flu in cows.
As for the milk, it was on its way to pasteurization. Even if the virus survived that (FDA later came out with a statement, and I agree, that it almost certainly will NOT), the milk would wind up in your highly acidic stomach, far from the respiratory cells it would like to infect. Your digestive process would most likely have finished what pasteurization started — with a small, but non-zero chance this might have primed your immune system for H5N1 bird flu if pieces of the dead virus were picked and shown to B-cells!
The reason to worry is not “virus in the milk — we iz all gonna get bird flu with our morning Cocoa Puffs”. The detection of H5N1 bird flu in so many milk samples means that lots of H5N1 got great chances to form Frankenflus in exposed cows.
The ability and opportunity to Frankenflu their way into something that CAN replicate in humans more easily, and spread human to human is the worry with bird flu.
“What about the 60% case fatality rate? Shouldn’t we still worry about that? Isn’t that the fear—bird flu Frankenflus to humans and brings -that- mortality rate with it?!?!?!” I hear you ask, Reasonable Question Hypothetical Reader.
Again, pump the brakes on that 60% CFR. Everyone cites the 60% mortality rate of confirmed bird flus in humans over the past several decades. Including, much to my annoyance, the “intro” sections of a lot of medical research papers on bird flu. That’s been published, so they can cite in the intros, sure. And it’s a good way to scare up grant money to keep doing research on bird flus (and we should be doing research on bird flus). The “60% mortality” citation is playing the game a bit, I get it.
But don’t believe that hype. The less-reported fact is that from July 2022 to July 2023, a total of14 people caught symptomatic bird flu.
Globally.
Only 2 died of disease. Now, 2 deaths in 14 symptomatic infections is still high, sure, but nowhere near 60%.
Moreover, and to reiterate, unless I have missed a more comprehensive screening in the literature, that “60%” calculation comes from studies and series that, at best, tested only symptomatic patients. I still very much suspect a lot of asymptomatic human cases have been out there, where a bird flu made it to their lungs, but could not replicate well if at all, and got stomped out by the immune system pretty quickly. That would actually be consistent with the studies in petri dishes showing that while only a few mutations are necessary for bird flus to get into human epithelial cells, they’re not very serious, rapidly replicating flus when there.
Now, all of that said, it is important to note that bird flu in birds can be incredibly lethal to birds. Some outbreaks have had 100% mortality of exposed birds. Crossovers as Frankenflus into some mammals have had some pretty serious flus as well.
“So what is going on in birds that bird flu nukes them — and is there any indication of that happening in the known human flu fatalities?” I hear you say, Hypothesizin’ Hypothetical Reader.
Necroscopy and lab studies in birds turns up some interesting findings. For example, a bird flu that annihilates geese in lab settings might only inconvenience ducks. So even among birds, there is some species-level variation that goes on. In general, in the ridiculously lethal bird flus, what vets have found is overwhelming numbers of the virus. The virus will not only replicate in the lungs of birds (so quickly it has taken the top off of some quantitative assays for the virus), but also nearly every other major organ. These bird flus are just exceptional at getting into bird cells, hijacking them, and cranking new flu viruses out at maximum effort.
Unfortunately, the data on the bird immune reaction to the really nasty bird flus is limited. Lab mammals exposed to the really nasty H5N1 bird flus show a strong inflammatory response in their lungs. In these mammals, that includes high levels of signaling molecules which tell the immune system and nearby “normal” cells to “start anti-viral procedures.” However, some of those same signals, if too active can tip over into sepsis.
So what we learn from birds and mammals is bird flus seem to kill birds by overwhelmingly high levels of viral replication, including replication in many different organs beyond the lungs. In mammals, we find they trigger an appropriate strong immune response to stop a virus (that, like any serious infection, can tip over into sepsis). In closely related mammals like pigs and primates, we find the virus can sometimes reach other organs outside the lung, but no evidence it replicates there, unlike birds.
Humans that die of bird flus have shown mostly acute respiratory distress syndrome with diffuse alveolar damage. That may be a rapid viral replication wipeout in the lungs — but you can also see that sepsis with multi-organ failure, which the human fatalities also overwhelmingly tend to have. Those patients where immune signal studies (cytokines) have been done show signals associated with sepsis. The viral strains involved are always some form of Frankenflu that is part human flu with a couple of the genes from the bird flu — typically an H or N, plus a few others.
One of the challenges in these human studies, though, is that the number of patients symptomatic, let alone killed, by any single Frankenflu strain is too small to know for sure if things like smoking history, underlying lung disease, underlying immune function, etc. are playing a role. Odds are good they are, but not enough cases at any one time to be sure. Again, there is not systematic testing of the asymptomatic close contacts also exposed to these Frankenflus to see if they were infected, but their immune system beat them. Odds are also good that has been happening — and probably a lot.
Given what we do know, to be a serious and scary pandemic, a bird flu would have to jump over to humans with that “replicate to liquidate ALL the organs” trick it does in birds. -Or-the bird flu would have to be really good at getting the immune system to go Ah-nold, similar to severe COVID. Since we haven’t really seen that widespread, organ liquidating viral replication we see in birds in mammals and humans, and petri dish studies are pretty consistent that bird flus which do cross over to infect human cells typically are not strong replicators, this seems to be a low probability. The bird flu’s other option — get the immune system to “guess wrong” or freak out and go full Ah-nold sepsis is probably how it would go. The likelihood of that is tough to handicap. Quite simply, having more robust screening of potential exposures, who may be or have been asymptomatically infected, would be a better measure of the rate at which a given bird Frankenflu breaking into humans is triggering sepsis overall, and a better measure of its true fatality rate.
We don’t have good data on that from previous outbreaks of cross over bird flus. Regardless, those past results would imperfect predictors of a future pandemic bird flu.
So . . . what to really watch for in news reports to know if a bird flu is breaking out and becoming a pandemic threat — to humans.
Obviously, you need to be reading about human cases. Lots of cows and ferrets turning positive for a bird flu is just a marker for a chance of Frankenflu. Most of the time, these do not cross over into humans, or more than a handful of humans at a time, who do not wind up spreading it person to person.
Remember that “first case announced in Australia”? If you stopped to read the article, that case was a child from India who travelled to Australia and came down with an admittedly solid case of the flu.
Back in March.
I’m not making that up. The headline and story is becuase Australia just finished the testing and confirmed the case as a bird flu.
None of that kid’s contacts caught a bird flu. There was no human-human transmission, and turns out, the kid was around a lot of birds in India before getting on a plane to Australia.
The US case likewise is a middle aged adult male working in the poultry industry. There is no evidence of human-human transmission in this case, and his flu was reportedly pretty mild.
Do more than your average investor (or algorithm) is doing and read the article. You are looking for human to human spread among contacts of confirmed patients, anyone catching bird flu who has NOT been around a bunch of (potentially sick) birds lately, and anything about underlying health conditions in the humans. Although somehow lay reporters hardly ever ask about other medical conditions in these patients, even though that is important. Lastly, look for human fatalities.
If there are any, they will not be hard to find.
“If it bleeds, it leads,” so if that handful of patients has any fatalities, that will get reported. Just remember — all initial estimates of the case fatality rate are much more likely than not to be way too high. This is because they are testing ONLY very severe cases, and very few patients overall. A few fatalities in a few cases is not statistically significant, but can get something that looks like “60% case fatality rate” pretty easy. You may recall in the first weeks of COVID-19 that fatality rates in that early reporting were up to 50%. Way too high an estimate — because the ability to test for SARS-CoV-2 specifically was rare and reserved for serious, highly symptomatic cases in the hospital. As that expanded to screening mild symptoms or no symptoms but contact with a known positive, we found the many more patients who were mildly affected or asymptomatic. Those are the true denominator, and the true case fatality rate of COVID was fortunately far, far less. So keep all of that in mind.
Start to worry more if you are reading about more new human cases in the following week or two.
You should really start paying attention if those “next few weeks” human cases are NOT in people who work with birds and animals a lot, and especially if you start getting new infections where the only known exposure was another positive case. That’s human-to-human spread, and that’s when we have a problem.
At that point, I’m probably back to regular weekly updates, where we will try to determine how worried to actually be.
Let’s close with a few points of optimism, and one note of caution.
Bird flus have been hovering around for a long, long time. They have caused pandemics in the past, true. The 1918 Spanish flu, for example, was a Frankenflu that had some avian origins — including an “H” that could bind human cells. However, a lot had to go right for the Spanish Flu, including an evolutionary incubator in the poor sanitary conditions of WW1 trenches, then back in packed field hospitals, where it selected for very rapid and deadly spread.
That’s actually important, and bears repeating.
The selection pressure matters. The 1918 flu took the turn it did because it was trying to spread in military hospitals. The host it invaded could very likely die from bullet, bayonet and artillary wounds — so a flu that could replicate as fast as possible (similar to the very deadly flus in chickens, for example) and get into new hosts as quickly as possible was favored. A flu replicating slower and more sneaky, and thus less deadly, might never have a chance in these densely packed hospitals. A rip roaring, deadly replicator near a LOT of new potential hosts would do much better — and did. That’s the 1918 flu pandemic.
Interestingly, as near as I can tell, the first highly pathogenic bird flu in birds (a “fowl plague”) was reported in Italy in 1878. Although not the factory-farming model of today, the industrial revolution was also changing approaches to agricultural practices. You can find a wide array of chicken coop styles from the 19th century here, with styles for just a few chickens on a small farm to some pretty massive palaces for mass production of eggs and chicken. Similar to a WWI field hopsital, though, if you have a bunch of hosts crammed together in close quarters, with occasionally questionable hygiene, you can foster a selection pressure on a flu virus that favors a “highly pathogenic” highly lethal, high replicating strategy. The flu doesn’t need to be sneaky — it has a lot of new hosts in close proximity. Now apply that to some of the modern “factory farming” techniques for chickens. Then give them the ability to transmit those to migratory wild birds who can now spread them farm to farm. I find it a really intriguing hypothesis, given the highest mortality rates for bird flus seem to be in domesticated birds with the necropsy evidence of a high replication strategy by the virus, if the way we keep chickens safe on farms is accidentally favoring these highly pathogenic bird flus…
Fortunately, for humans at least, we do not have the same kind of conditions as say, WWI field hospitals for our average flu to get that kind of evolutionary amplifier.
In fact, the Spanish Flu is an exception, not the rule, with bird Frankenflus. Despite many opportunities every year to make the proverbial leap, they haven’t. You get a handful of cases that cause symptoms in humans, and most of those do not spread person to person. The odds of such a Frankenflu emerging in any given year are not zero — there will always be a chance it could mix and match its way to pandemic. But the preponderance of history suggests those odds are not high, either.
Further, ever since 1918, we are more prepared for flu. We have several already approved medications that can hit flu at multiple stages of its replication cycle. How well, or if, and how many of them will work against an emergent bird Frankenflu pandemic is unknown until the actual virus emerges. But we do have several shots on goal sitting on the shelves already, and it is unlikely a new pandemic virus will naturally dodge them all. We also have vaccines, which are updated seasonally already, with a long history of experience in manufacture, distribution and potential side effects of flu vaccines (very minimal). A close enough “guess” to an emergent pandemic flu with a vaccine may well be enough to end the pandemic threat it poses, be it direct mortality or “bed’s taken,” similar to COVID.
The note of caution in our ability to treat and vaccinate is more social than anything. Even though the start of the COVID pandemic is already 5 years behind us (really!), the damage to trust in institutions remains. The disastrous COVID vaccination campaign, in particular, has already led to epidemics of mumps and measles as more people question the value of all vaccines. There is already a significant proportion of the population that does not get a seasonal flu vaccine. Even if a flu pandemic happens, because of the institutional mistakes that were made, and I believe remain uncorrected, vaccine and treatment adoption will be reduced. I don’t think that will change for a long time — probably a generation or more.
During COVID, institutions convinced themselves they were telling the “good lie” with many pronouncements and policies, and they sometimes compromised scientific integrity to do that. People neither tend to forget nor easily forgive those who lie to them, especially in times of crisis. No matter the intention behind it. Thus, we risk the whirlwind harvest from the seeds the “well-intentioned” sowed.
Only time, and leadership aimed at restoring virtue and trust, will change that.
So what are your chances of catching a pandemic bird flu?
Our regular readers are well-accustomed to seeing how tiny events, small shifts, can transform into dire inevitability.
Thus, our regular readership will recognize the following video for what it really was:
One of the greatest mistakes in human history.
Yes, that was the tragic moment where tourists in Bali, not knowing the consequences, or the stakes involved, negotiated with a member of the Army of the Bioterrorist Monkeys.
Never negotiate with bioterrorist monkeys.
Never.
This taught the Army of the Bioterrorist Monkeys that humanity is weak where our technology is concerned, and if they can secure our communications and computers, they can extract concessions from us.
A new front has been opened. A new arms race.
Is it any surprise, then, that we have read headlines since this event of highly organized, skilled hackers taking over pharmacy ordering systems, paralyzing distribution of medication? Or ransomware events at major health insurers and hospital systems?
You thought it an accident that healthcare technology systems have been impacted — as if healthcare infrastructure were not a primary target of the Army of the Bioterrorist Monkeys?
Official sources have not named the organizations behind many of these headline hacks. Of course not. The conflict with the Army of the Bioterrorist Monkeys has ever lurked in the shadows, lest the enormity of the true danger become clear. But now you know why you can never, never negotiate with bioterrorist monkeys — and how that innocent mistake has led to the rise of the cyber division of the Army of Bioterrorist Monkeys, and the hot cyber war humanity is now engaged in.
(original creation via DALL-E3 model on NightCafe)
You may also think that sudden explosion of AI and robotics and concern of “arms races” for military and intelligence applications of these technologies is an all too human story of nation versus nation, company versus company, tribe versus tribe.
This, as usual, is only part of the truth. There is an arms race in these technologies, true. An arms race that we, humanity, must win — to secure our future, our planet, our species. One in which many nations are already fully engaged.
Yes, the Army of the Bioterrorist Monkeys cyber division’s ransomware attacks are funding a robust program of offensive, primate directed AI and robotics.
Fortunately, humanity holds a tenuous lead, developing AI and robotics to counter the Army of the Bioterrorist Monkey threat…
As I write this, right now, your chances of a human bird flu pandemic are equivalent to the chances of the Army of the Bioterrorist Monkeys against humanity’s greatest champion -- now that Dr. Jane Goodall has been cybernetically augmented to take the battle to the monkeys. In whatever reality they choose.
(Original creation with NightCafe Stable Core model)